Preparing to meet the needs of infants and children impacted by emerging threats requires an entire system approach. This graphic provides a visual tool to help support conversations in communities and to identify elements within the system of care that can be strengthened to ensure the needs of infants and children are met when faced with an emerging threat or disaster.

Overview
The American Academy of Pediatrics (AAP), with support from a cooperative agreement with the Centers for Disease Control and Prevention (CDC), leads a project to educate and collaborate with pediatricians, families and community partners to protect infants and children from emerging threats. Under this cooperative agreement, the AAP gathered experts representing a variety of perspectives – including pediatrics – to inform the development of a visual representation that depicts the characteristics for a system of care that can effectively support infants and children impacted by emerging public health threats.
In February 2024 subject matter experts across multiple disciplines, including pediatricians, public health partners, and families with lived experience participated in focus group sessions to provide input on the current system of care graphic, as well as insight into avenues for improving access and outcomes for those entering and working withing the system. Information from these sessions was used to inform a larger system of care meeting, consisting of varying subject matter experts collaborating within a single forum, aiding in updating the system of care graphic.
This updated graphic is reflective of the lessons learned from the COVID-19 pandemic and provides a visual representation of the characteristics of a system of care that can effectively support infants, children and families impacted by emerging threats. A conceptualization of the elements necessary to meet the needs of families accessing the system of care, the goal for this graphic, is utilization as a tool for pediatric health professionals, community partners and the public health workforce to aide in the identification of gaps and development of strategies that allow for implementation of the identified elements for an effective system of care.
Themes Identified
Themes identified in the focus groups meeting informed the System of Care meeting and aided in the development of the updated system of care graphic. Below are the themes which provided the foundation for identifying the elements for an effective system of care.
- Families are Central
- Partnerships are Vital
- Effective Communication is Key
In addition to the three themes identified, it was also noted that families enter the system of care at varying points. Access to the system is impacted by a myriad of factors inclusive of - but not limited to - social drivers of health, lack of equity, transportation, insurance, legislation, and collective burnout of health care staff and society overall.
Designed with Families
Recognizing the multitude of factors impacting the system of care and the systemic challenges that play a role in how families access health services, a graphic depiction of the elements of an effective system of care was conceptualized. Considering the many ways families access health services, this graphic provides a visual representation of the varying partners in health encountered by families and identifies elements poised to assist in the coordination and connection of health services across the system. Designed with families, this graphic depiction identifies foundational elements for “Building a system of care that protects infants and children from emerging threats”.
Family Focused

Families are the driving force for the system of care. Ideally, the individual components of the system of care work together to meet the needs of infants and children impacted by emerging threats through engaging the whole family. Without families leading the way, the system cannot operate as intended; the family voice is vital in building a system of care that is poised to meet the needs of infants and children impacted by an emerging threat.
With this in mind, the graphic was developed with leadership and input from families with lived experience. They provided insight into their experience navigating the system, the challenges that were faced during COVID-19 and the elements that could aid access to care when facing an emerging threat.
Progress in Partnerships
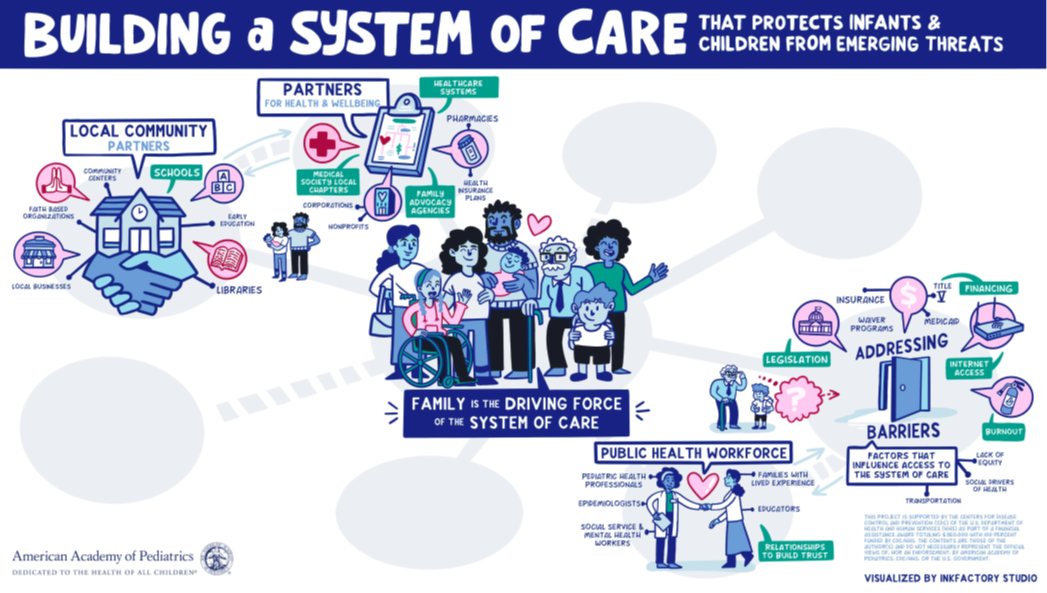
Health partners play a vital role in a family’s access to health services. These partners are inclusive of but not limited to local community partners (schools, libraries, local businesses, faith-based organizations, etc), partners in health and wellbeing (pharmacies, healthcare systems, nonprofits, family advocacy organizations, etc) and the public health workforce (pediatric health professionals, epidemiologists, educators, social services, etc).
As discussed, families access health care in many different ways, and the role of health partners in the provision of health services can vary depending on the community serviced. Access to care and the delivery of health services for infants and children can be impacted depending on partner interaction within the system of care. Health partners working together can address barriers to care; when those same health partners do not collaborate effectively, additional barriers are introduced if the appropriate elements are not in place. Recognizing the vital role of engaging health partners across the system of care, ensuring access to necessary elements can both strengthen partnerships and provide a foundation for building an effective system of care.
Connection through Communication

Effective communication is key to the continuous interaction of all the components that make up the system of care. Identifying key elements that can aid in connecting families and partners across the system of care is critical to providing the foundations for building an effective system of care that protects infants and children from emerging threats. Connection across the system of care helps to identify gaps in services and address barriers impacting access to care. A key element in developing that connection is implementation of effective communication across the system of care. Effective communication is multidirectional, data informed, timely, culturally inclusive and consistent. Implementation of elements such as data sharing agreements, coordinated referral systems, care coordination and continuous feedback loops establish ongoing correspondence which strengthens communication during times of crisis. Effective communication aids in building trust and addressing dis/misinformation. Implementing elements that strengthen communication with families and health partners across the system of care supports connection to services, provides a coordinated approach to care, creates avenues to address barriers and implements a process for continuous improvement.
Video: Building an Effective System of Care to Address Emerging Threats to Infants and Children
The video below shows how the system of care graphic can be used by advocates, families and community health partners to support a system of care that can meet the needs of infants and children impacted by an emerging threat. As identified by families and health partners the elements depicted aid in addressing barriers to health services and establish an avenue for building the foundation of an effective system of care. Intended for use as a visual tool, the graphic aids in identifying gaps in care and the elements needed to address barriers and improve access to services. Building towards a collective goal, this system, driven by families, strengthened with partners and connected by communication progresses forward. The video below envisions this goal, a system of care, inclusive of all of these elements. It serves as a visual tool for family and health partners to open dialogue, collaborate, and initiate steps that aid in building an effective system of care that is ready to meet the needs of infants and children when an emerging threat arises.
This project was supported by the Centers for Disease Control and Prevention (CDC) of the U.S. Department of Health and Human Services (HHS) as part of a financial assistance award totaling $250,000 with 100 percent funded by CDC/HHS. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by American Academy of Pediatrics, CDC/HHS, or the U.S. Government.
Last Updated
02/19/2025
Source
American Academy of Pediatrics