There have been concerns about how the COVID-19 pandemic and subsequent shelter-in-place orders have affected risk for intimate partner violence (IPV) within the United States and abroad. IPV is harmful to both the adults who experience it and to children in the home who witness IPV. Additionally, as reported in a prior snapshot, parents who are experiencing IPV are also more likely than others to report that they are spanking their children. In this snapshot, we present findings about IPV among adults in the home.
IPV describes “physical violence, sexual violence, stalking, and psychological aggression by a current or former partner or spouse (ie, boyfriend/girlfriend, dating partner, or ongoing sexual contact partner).” The Family Snapshot Survey included standard questions about IPV sourced from the CDC’s Violence Against Children Surveys (VACS). Four items on physical violence included behaviors like slapping, pushing, kicking, punching, beating, choking, burning, and threatening with or using a weapon. Five items on psychological violence included things such as insulting, humiliating, withholding access to money, restricting access to family/friends, tracking activities and whereabouts, and threatening to harm the person. It is important to note that this survey did not include questions on stalking or sexual violence.
Key Messages
- Intimate partner violence was concerning during the pandemic – 1 in 5 adult respondents reported experiencing IPV, including 11% who reported experiencing physical violence. Both men and women reported IPV. Providers should ask both male and female parents about IPV in a private setting away from their partner, their children, family members, and friends.
- Witnessing IPV is an adverse childhood experience (ACE) and can have harmful effects on mental, physical, and behavioral health across a child’s lifespan. Pediatricians and pediatric healthcare providers should be aware of the rates of IPV reported during the pandemic and the potential effects on children.
- Families who are experiencing economic or psychological distress reported higher rates of psychological and physical IPV. Resources offered to stressed families might include community based IPV resources, allowing adults to access these resources as needed.
- If families report that they have spanked their children, an inquiry into adult safety in the home is appropriate, because IPV was far more common in homes where children were spanked (61% vs 13%).
One in 5 respondents (21%) reported that they have experienced physical and/or psychological IPV since the beginning of the COVID-19 pandemic (March 2020). This number includes 2% who reported experiencing only physical violence, 11% who experienced only psychological violence, and 8% who experienced both physical and psychological violence. It is important to note that this sample was comprised of parents with children in the home, which means that in 21% of the households sampled, children were potentially witnessing IPV during the pandemic. This is important because witnessing IPV is an ACE and can have harmful consequences across the lifespan for children.
Both men and women report experiencing psychological and physical IPV. When reporting on experiences of IPV since the beginning of the pandemic, higher percentages of men report experiencing both psychological IPV only (13%) and physical IPV (with or without experiencing psychological IPV; 14%) than women (8% psychological only and 8% physical, +/- psychological).

Emotional IPV includes being insulted, humiliated, having money withheld, restricted access to family/friends, being tracked, or threatened by an intimate partner.
Physical IPV includes being slapped, pushed, kicked, punched, beaten, choked, burned, or threatened with or having a weapon used against you by an intimate partner.
The proportion of men and women experiencing physical IPV since the beginning of the pandemic is substantially higher than previous past-year estimates for men and women. In the 2015 National Intimate Partner and Sexual Violence Survey (NISVS), approximately 4% of men and 3% of women reported physical IPV in the last 12 months (NISVS did not report 12-month prevalence of psychological IPV). Although the sample for this survey is not directly comparable to the NISVS sample, it is notable that greater percentages of men and women were reporting physical IPV in the approximate 9 months since the pandemic began than were reporting physical IPV in a nationally representative sample in the past 12 months in 2015. The finding that higher percentages of men than women were reporting IPV during the pandemic warrants further investigation.
Reports of lifetime experiences of IPV in the sample for this survey reflected similar reports between men and women, which is consistent with national surveys. In the sample, 19% of men and 13% of women report experiencing only psychological IPV, and 25% of men and 28% of women report experiencing physical IPV (+/- psychological IPV). These similarities by sex in the findings are consistent with 2015 NISVS estimates of lifetime experiences of IPV: substantial and similar numbers of men and women reported experiencing physical (31% for both) and psychological (34% of men and 36% of women) IPV in their lifetimes. The NISVS estimates also demonstrated that greater percentages of women than men experience sexual IPV and stalking IPV, and greater percentages of women than men report some form of IPV-related impact like injury or missing days of work, none of which were measured in our survey.
It was not possible to determine from this survey whether IPV rates had changed during the pandemic. Altogether, less than half (42%) of adult respondents had ever experienced violence within their intimate relationships. Of these, about half (54%) reported that they were not currently experiencing it since March 2020 or during the pandemic.
IPV and stress
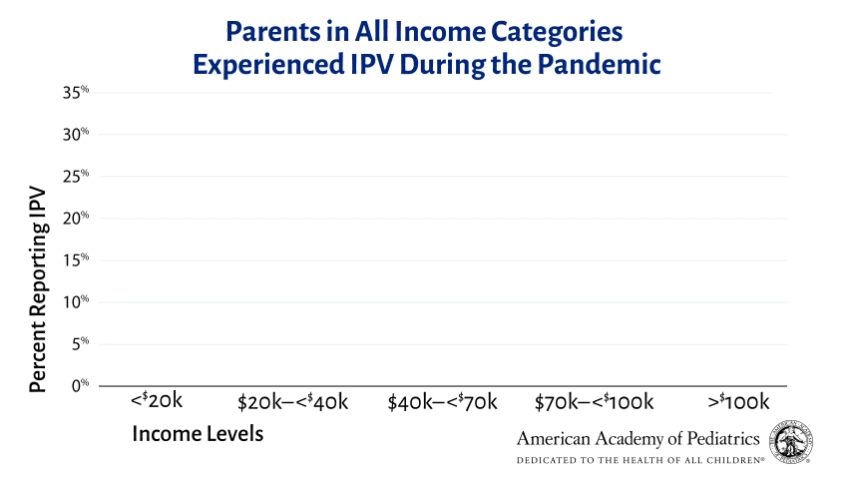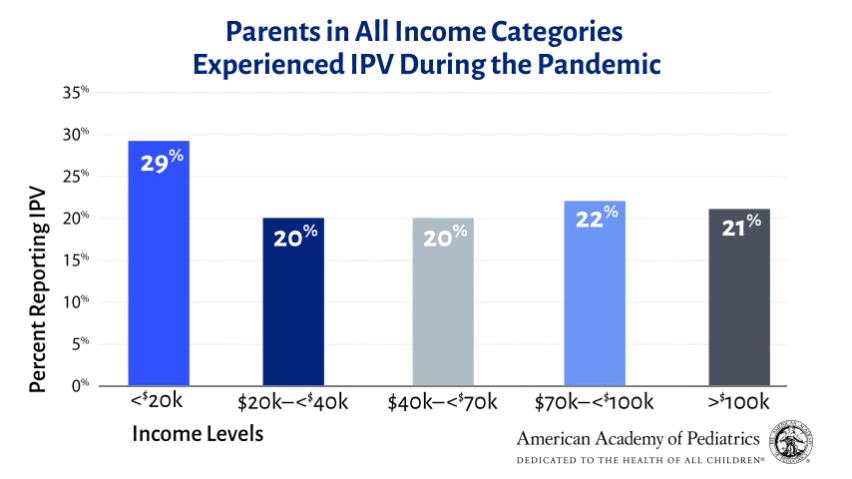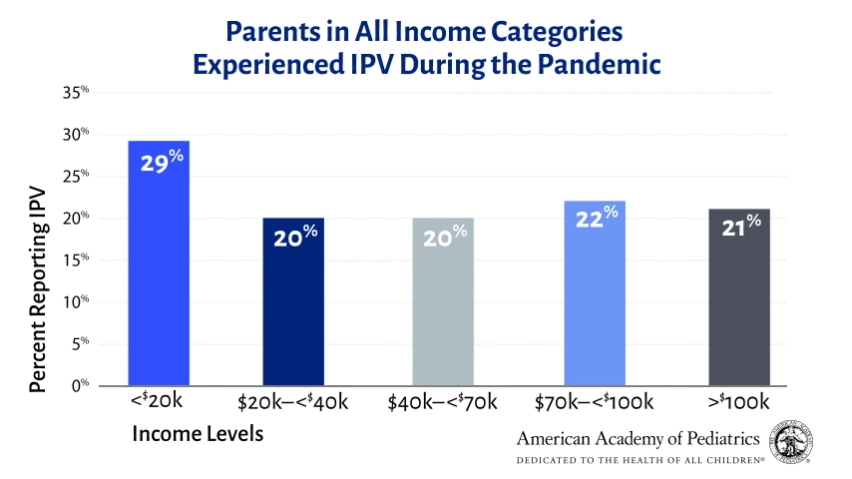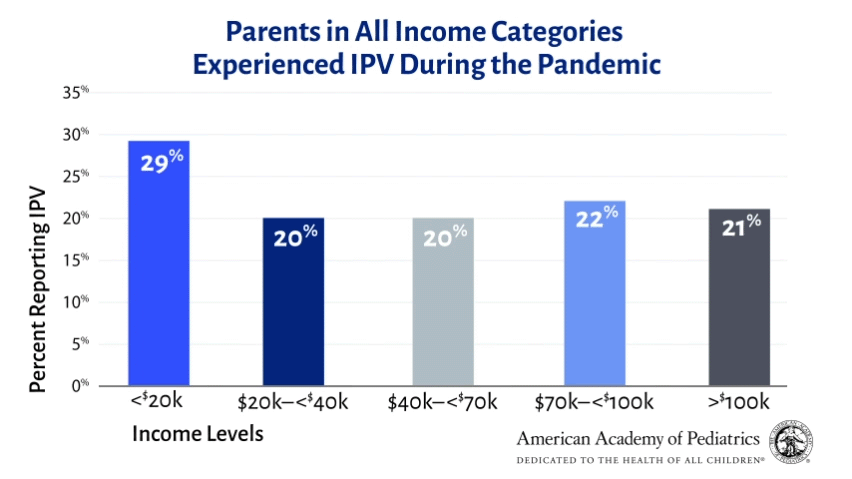
Reports of IPV appeared high across all income levels (see figure). However, stressors that may have been exacerbated during the pandemic were associated with higher rates of IPV. In particular, financial stress was associated with reported IPV: Respondents with lowest family incomes (16% of all families, income less than $20,000) reported the highest rates of IPV since the beginning of the pandemic (29%). This is consistent with prior research finding that stress, and financial stress in particular, puts people at higher risk for IPV.
Emotional stress and unhealthy coping strategies were more common when IPV was reported. More people who reported IPV during the pandemic also reported feeling nervous or stressed all or most of the time or that difficulties were piling up so high that they could not overcome them compared with those who did not experience IPV (26% vs 18%). In addition, more people who reported IPV during the pandemic also reported less healthy coping strategies (alcohol, smoking, or other drugs) than those who did not report experiencing IPV (32% vs 15%).
A few things are important to keep in mind when interpreting these results. First, as noted above, this survey’s measure of IPV does not capture sexual IPV, stalking, or the impacts of the IPV, making it particularly hard to interpret the differences between men and women in experiences of IPV. Additionally, some of this survey’s measures of psychological IPV may have been experienced and interpreted in a different context given conditions of the pandemic. One kind of emotional IPV occurs when “a partner tries to keep you from seeing or talking to your family or friends.” It is difficult to know whether social distancing and other restrictions resulting from the pandemic may have influenced how people answered this question. Providers may consider asking about how individuals have maintained contact with their support networks during the pandemic. Although social distancing protects physical health, it is important to distinguish protective behaviors from controlling behaviors.
IPV has long-term effects on both the physical and emotional health of children. Pediatricians can play an important role in identifying IPV by performing targeted screening of families at high risk for IPV or screening all families in their care for IPV. Pediatricians should consider the needs and safety of children and the parent experiencing IPV and provide collaborative trauma-informed support and referral.
Resources for Pediatricians
Resources for Parents and Caregivers
Last Updated
06/08/2021
Source
American Academy of Pediatrics