For the best health outcomes, the AAP recommends exclusive breastfeeding for approximately 6 months followed by continued breastfeeding with complementary foods for at least 2 years and beyond as mutually desired.
The AAP provides detailed information on breastfeeding and breastfeeding support for clinicians that includes
- Physician education and training
- Breastfeeding practice tools for health professionals
- Training curriculum for residents
- Workplace support including legal information
- Model policy for medical, resident, and fellowship trainees to advocate for supportive breastfeeding policies for medical trainees
- AAP local chapter contacts
- Donor milk drive toolkit
- Informational podcasts
- Milk storage guidelines
- Comprehensive list of breastfeeding policies and recommendations from the AAP and other policy-setting organizations
The Benefits of Breastfeeding
Human milk has leukocytes and antimicrobial, antiinflammatory, and immunoregulatory agents, which aid the developing immune system of the child.
Six months of exclusive breastfeeding is associated with decreased rates of lower respiratory tract infections, severe diarrhea, otitis media, and obesity, among other outcomes.
Breastfeeding and Infant Outcomes
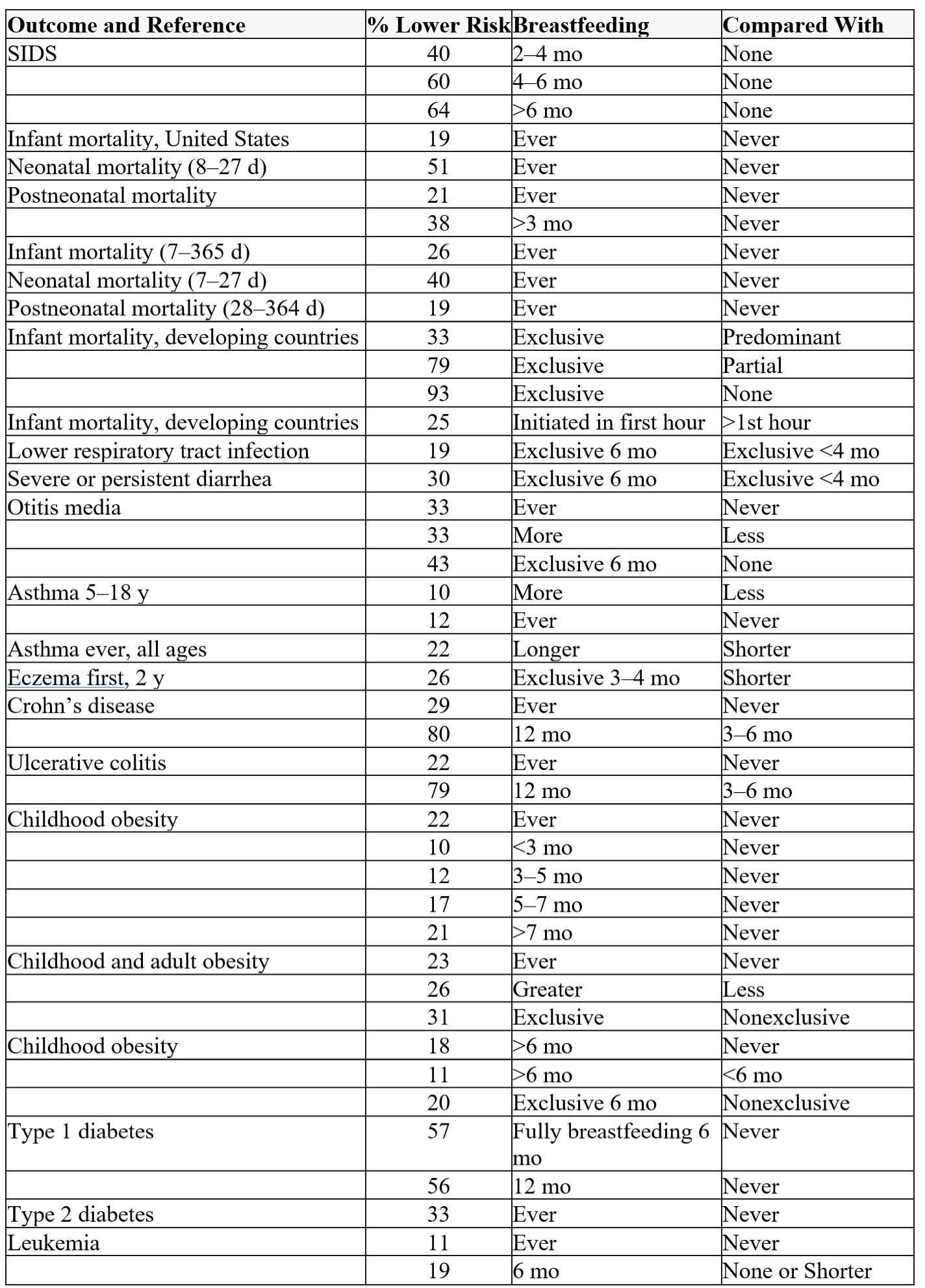 SIDS, sudden infant death syndrome.
SIDS, sudden infant death syndrome.
Excerpted from: Breastfeeding and the Use of Human Milk
In addition to benefitting infants, breastfeeding offers
- Societal benefits
- Environmental, in that it doesn’t require manufacturing.
- Parents miss less work because breastfed babies are not sick as often.
- Maternal benefits
- Reduced risk for excessive bleeding during menstruation
- Reduced risk for several diseases such as
- Rheumatoid arthritis
- Hypertension
- Type 2 diabetes
- Certain cancers
Breastfeeding the Newborn
National efforts to promote breastfeeding have driven improvements in breastfeeding initiation rates. The US national average for breastfeeding initiation is approximately 84%. However
- By 3 months only 47% of mothers are exclusively breastfeeding, and this rate drops to 27% at 6 months.
- Of babies born in 2019, approximately 1 in 6 did not receive any human milk. (ref)
- Breastfeeding initiation rates are generally higher among infants of Asian and white mothers and lower among Black and American Indian/Alaska Native mothers, although this is not true in all states. (ref)
- Breastfeeding disparities are often state specific.
- Check updated breastfeeding data by state at the Centers for Disease Control and Prevention interactive trend map.
Pediatrician’s Role in Breastfeeding
- Pediatricians should review the importance of exclusive breastfeeding, ensuring mothers and families are fully informed.
- Engage in nonjudgmental conversations about the family’s personal goals for breastfeeding. Exclusive breastfeeding is not always possible.
- Encourage open communication and avoid language that may shame a mother who is unable or unwilling to breastfeed.
- Women reported significantly greater comfort discussing their decision to breastfeed beyond 1 year with family members and close friends than with their child’s primary care professional, and approximately half of mothers who breastfeed beyond 1 year do not discuss this decision with their child’s physician.
- 38% of women elected to change their pediatric primary care professional because they perceived a lack of support for breastfeeding >1 year.
The pediatrician’s role in breastfeeding initiation is critical. Pediatricians should
- Promote breastfeeding as the norm for infant feeding.
- Recommend exclusive breastfeeding for approximately 6 months.
- Encourage continuing breastfeeding until at least 12 months of age and up to 2 years or beyond if mutually desired.
- Add complementary foods at approximately 6 months of age.
- Educate parents about the importance of human milk for all infants.
- Human milk and its components.
- Benefits of breastfeeding.
- Correct any false beliefs about infant feeding.
- Prepare mother for hospital experience and recommend that
- Baby goes skin to skin at delivery.
- Routine nursery care and preventive treatments may be delayed until after the golden hour to allow for first nursing.
- 24-hour rooming-in is practiced.
- Elective procedures (eg, bathing, circumcision) are delayed until newborn is feeding well.
- Encourage unrestricted nursing on demand, at least 8 to 12 times per day.
- Educate parents about recognizing hunger cues.
- Unnecessary supplements should be avoided even after breastfeeding is well established; pacifier can be introduced after breastfeeding is well established.
- Address parental questions and concerns.
- Avoid any promotion of commercial infant formula or feeding equipment in the hospital or office.
- Implement breastfeeding-supportive office practices.
Establish office practices that support breastfeeding.
- Have a written breastfeeding-friendly office policy.
- Train staff in breastfeeding support skills.
- Discuss breastfeeding during prenatal visits and at each health supervision visit.
- Encourage exclusive breastfeeding for 6 months.
- Provide appropriate anticipatory guidance that supports the continuation of breastfeeding as long as desired.
- Incorporate breastfeeding observation into routine care.
- Educate mothers on breast milk expression and return to work.
- Provide noncommercial breastfeeding educational resources for parents.
- Encourage breastfeeding in the waiting room but provide private space on request.
- Eliminate the distribution of free formula.
- Train staff to follow telephone triage protocols to address breastfeeding concerns.
- Collaborate with the local hospital or birthing center and obstetric community regarding breastfeeding care.
- Link with breastfeeding community resources.
- Monitor breastfeeding rates in your practice.

The development of this resource was made possible with support from Abbott. The AAP maintains full independence in its editorial and strategic activities. Financial supporters have no influence over AAP content, policies, or leadership decisions.
Last Updated
02/13/2026
Source
American Academy of Pediatrics
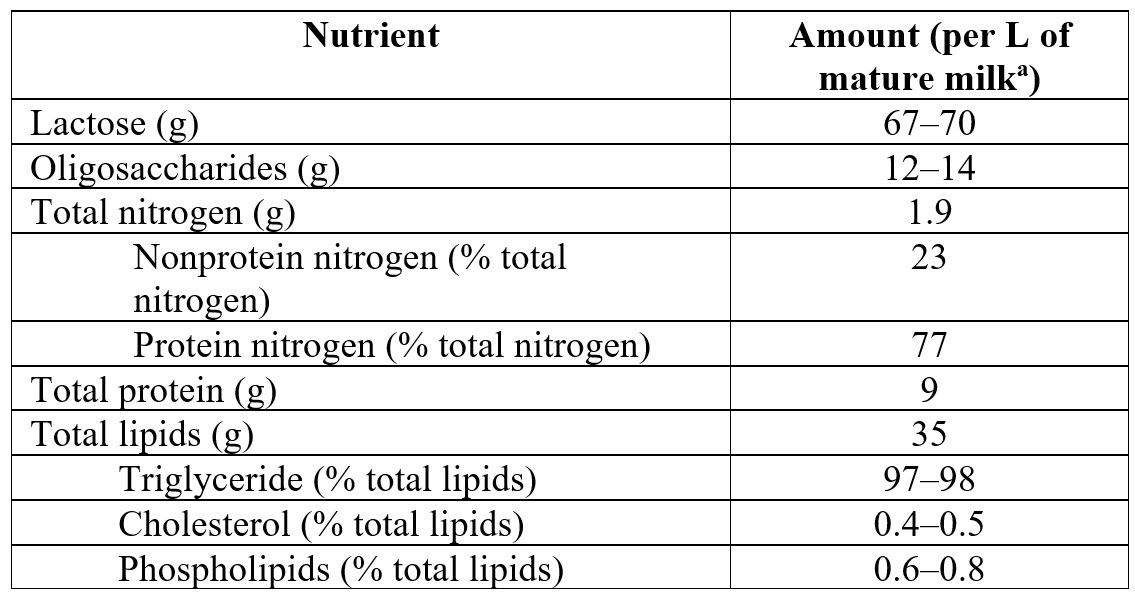 a Mature milk = after 2 weeks’ lactation.
a Mature milk = after 2 weeks’ lactation.