Chloe Somberg, William Burr, Janet Lee, Maria H. Rahmandar, Suzanne Rybczynski
Presented at the 2026 Pediatric Academic Societies Annual Meeting
Background: Suicide is the 2nd leading cause of death among US youth beginning at age 10. In 2022, the AAP and American Foundation for Suicide Prevention published the Blueprint for Youth Suicide Prevention, outlining strategies for clinical settings. National data are needed on primary care pediatricians' current experiences caring for youth with suicidal ideation.
Objective: Examine primary care pediatricians' experiences managing patients’ suicidal ideation.
Methods: 2025 Periodic Survey, a national random sample of non-retired US primary care AAP members, queried experiences with patient mental health including a) frequency pediatricians care for patients with suicidal ideation, b) risk assessments and care plans used when patients present with suicidal ideation and c) comfort discussing suicidal ideation with patients and families. Response rate was 46%; analytic n=801, includes those providing health supervision. Chi-square tests examined the association between caring for patients with suicidal ideation (bifurcated as: every day/few times a week/once a week vs once a month/few times a year/never) and practice characteristics (area, setting, US region, practicing at a federally qualified health center, patient financial hardship, insurance source, patient race and ethnicity).
Results: Nearly all (98%) primary care pediatricians reported ever having a patient present with suicidal ideation. 57% reported caring for patients with suicidal ideation at least monthly, with 23% reporting at least weekly. Among pediatricians who ever had a patient with suicidal ideation, over 90% always “find out if the patient already established care with a mental health clinician” and "assess if the patient has a plan to die by suicide" when a patient presents with suicidal ideation, with additional assessments and care plans noted in the figure. Most reported being very comfortable (23%) or comfortable (47%) discussing suicidal ideation with patients and their families.
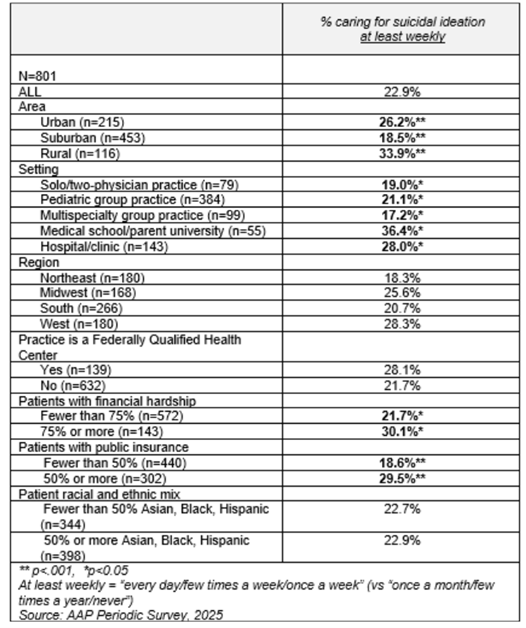
Caring for patients with suicidal ideation at least weekly varied significantly by practice area, setting, patient financial hardship, and insurance source [Table]. For example, pediatricians in rural practices were more likely than those in urban or suburban practices to report caring for patients with suicidal ideation at least weekly (34%, 26%, 19%, respectively).
Conclusion: The majority of primary care pediatricians report caring for patients with suicidal ideation and always providing risk assessments and care plans to support these patients. Pediatricians in rural and under-resourced practices report higher rates of patients with suicidal ideation.
Figure 1. Risk Assessments and Care Plans Used by Primary Care Pediatricians for Patients Who Have Suicidal Ideation
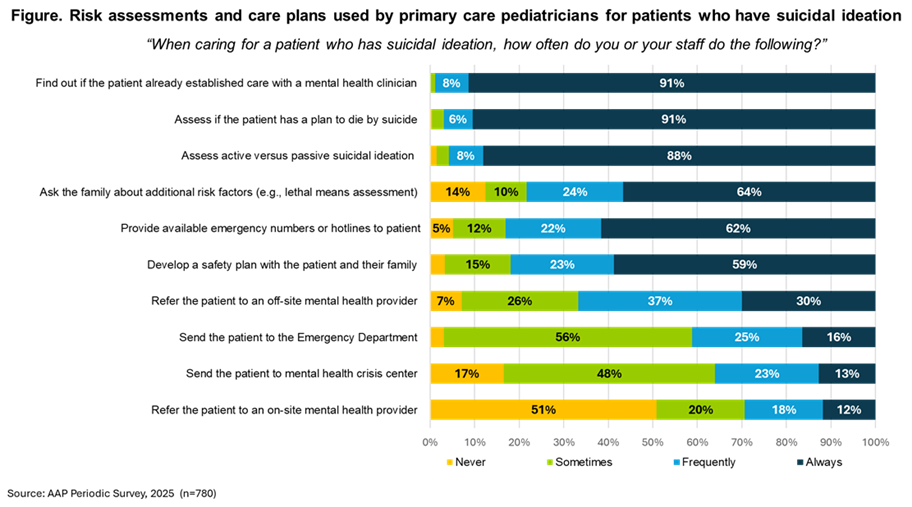
Table 1. Association Between Primary Care Pediatricians’ Reported Frequency of Caring for Children with Symptoms of Suicidal Ideation and Practice Characteristics
Last Updated
05/05/2026
Source
American Academy of Pediatrics