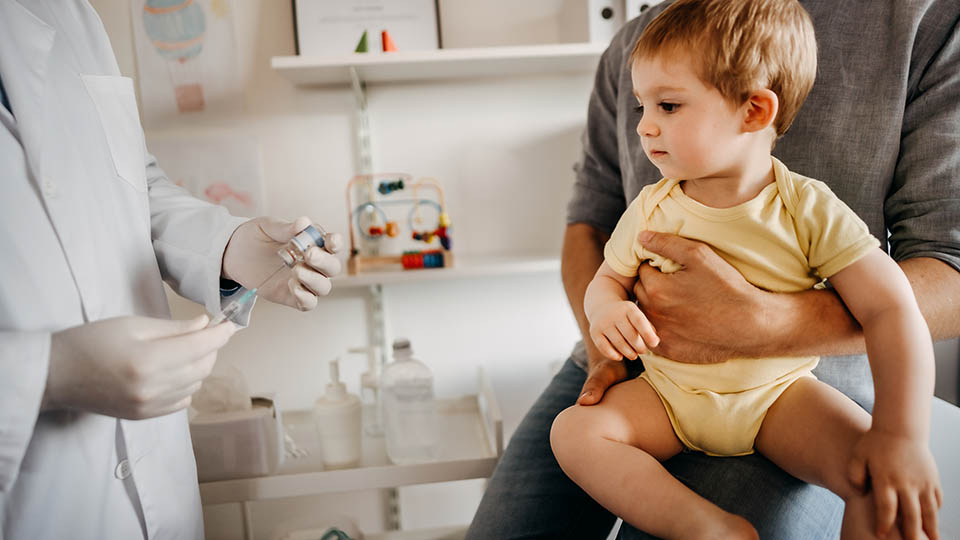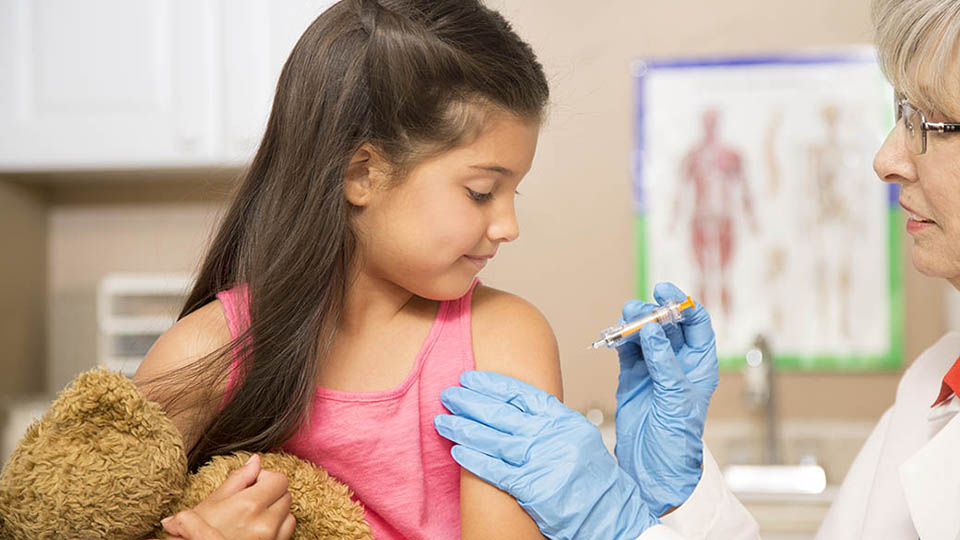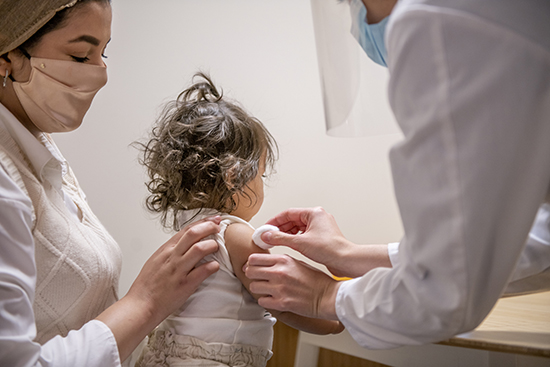

View the recording of COVID-19 Vaccines: Clearing the Air on Liability and Practice Considerations to hear from legal, clinical and communication experts on shared decision-making and professional protections for administration of COVID-19 vaccines to children.
COVID-19 Overview
COVID-19 (coronavirus disease 2019) is a disease caused by the SARS-CoV-2 virus. COVID-19 most often causes respiratory symptoms, although some people can become severely ill.
AAP Recommendations
The AAP recommends routine vaccination against COVID-19. Specific information on how to prevent, diagnose, and treat COVID-19 can be found in the COVID-19 Chapter of the AAP Red Book.
More About the Science
The vast majority of Americans have some immunity to COVID-19 either though immunization, infection, or both following the global pandemic (2020-2023). However, immunity wanes over time as the virus mutates. COVID continues to cause hospitalization and death in pediatric populations with rates of COVID hospitalization highest among infants who are less than 6 months of age. Additionally, some infected people will go on to experience long-term symptoms known as Long COVID.
Professional Tools & Resources
Lessons Learned from the COVID-19 Pandemic
Resources for Families
View this collection of COVID-19 articles written for the patient and family audience.
Get Involved
Last Updated
12/11/2025
Source
American Academy of Pediatrics