Frintner MP, Somberg C, Haftel H
Accepted for 2020 Pediatric Academic Societies Annual Meeting
Background: Pediatric subspecialty fellowships are common pathways for graduating pediatric residents. While some subspecialties continue to grow, others struggle to fill their spots.
Objective: Examine factors of importance in residency graduates decision to pursue fellowship by resident characteristics.
Methods: A random sample of 1000 residency graduates across all US programs via the 2019 AAP Annual Survey of Graduating Residents were surveyed. Residents were asked about their plans after residency and importance of 12 factors in the decision to pursue their specific fellowship. Chi-square examined variations in importance (essential or very important vs somewhat or unimportant) by gender, have children, medical school location, education debt, location of residency training and program size.
Results: 504 (51%) responded. 189 (38%) reported they would be starting pediatric subspecialty fellowships following residency. Majority of these residents reported starting training in neonatology (16%), hematology/oncology (14%), cardiology (12%), emergency medicine (10%) or critical care (9%).
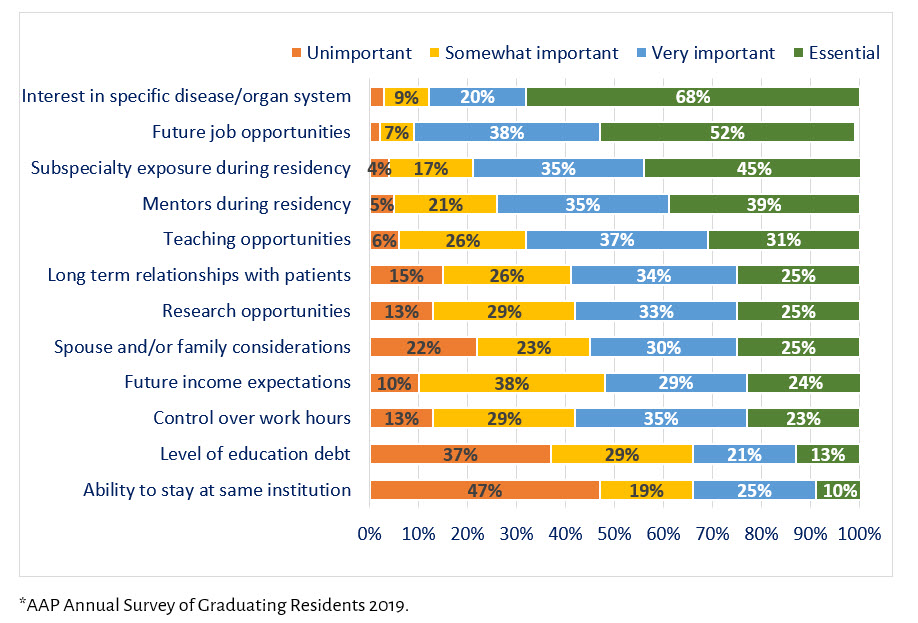
Regarding factors of importance in decisions to pursue fellowship (Figure 1): future job opportunities and interest in specific disease/organ system were the 2 highest rated factors, with most reporting them as essential or very important (90% and 88%, respectively). Other important factors included subspecialty exposure and mentorship during residency. Factors with the lowest ratings were ability to stay at same institution and education debt, with 1/3 reporting essential or very important.
No variation in factors of importance was found by gender, region and program size; few were found by medical school location and debt. For example, 93% of residents from US and 81% from international medical schools reported job opportunities to be essential or very important in their decision, p<.05. Most variation was found among residents with children. For example, residents with children were more likely than those without to report family considerations and control over work hours as essential or very important (86% vs 48%, p<.001; 80% vs 53%, p<.01, respectively).
Conclusion: Four in 10 graduating residents report starting fellowship training after residency. Residents similarly prioritize factors important in choosing their subspecialty across gender, region and program size, with top factors being job opportunities and interest in specific disease/organ systems. Family considerations and control over work hours are particularly important for residents with children.
Figure 1. Factors Important in Decision to Pursue Specific Subspecialty: Percent Reporting Among Graduating Pediatric Residents, 2019 (n=188)*
Last Updated
10/08/2021
Source
American Academy of Pediatrics