Gottschlich E, Frintner M, Fiks A
Presented at the 2023 Pediatric Academic Societies Annual Meeting
Background: The AAP declared a national emergency in children’s mental health in 2021. Current data are needed on pediatricians’ experiences addressing mental health needs across practice areas.
Objective: Describe primary care pediatricians’ views on and experiences addressing child mental health needs and examine variation by practice area.
Methods: National weighted survey data from 3 AAP Pediatrician Life and Career Experience Study (PLACES) cohorts: 2016-18, 2009-11 and 2002-04 residency graduates. Data were collected in 2022 (response=67%). Analytic sample (n=749) restricted to primary care pediatricians (PCPs). Respondents reported views on and experiences addressing child mental health needs: mental health is a problem currently (not at all to significant problem); concern compared to before pandemic (much less to much more concerned); resource availability (not at all to very available); frequency caring for anxiety, depression, eating disorders, suicidal ideation/behavior (never or a few times a year to every day); difficulty finding care for patients (not at all to very difficult); prescribe psychotropic medication (yes/no); and comfort prescribing (not at all to very comfortable). Chi-square examined variation in views and experiences by practice area (inner city/urban/suburban/rural).
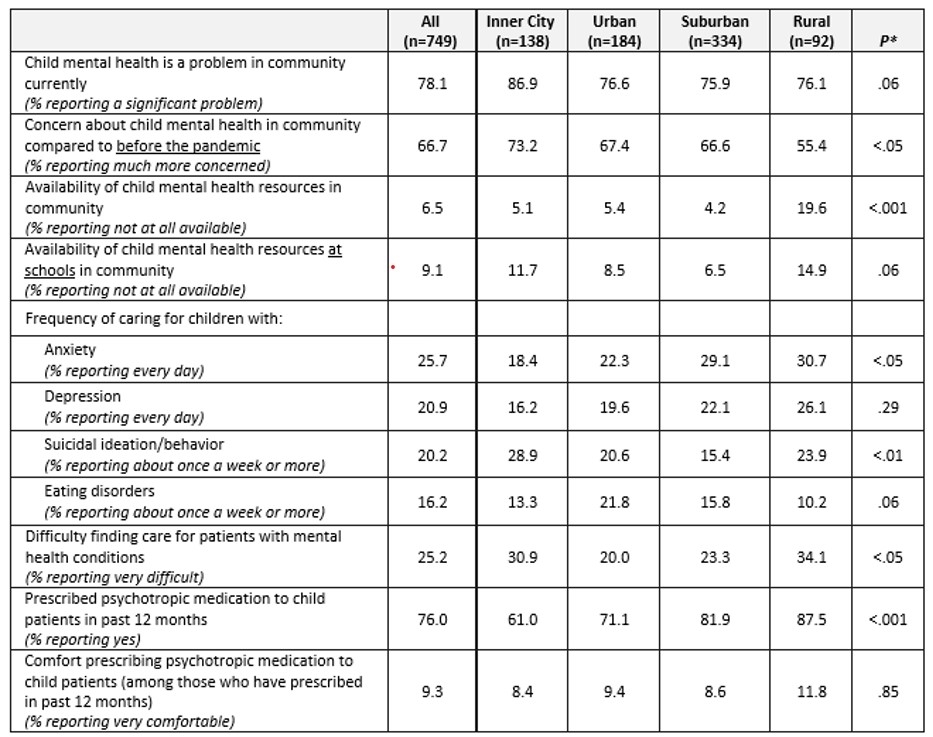
Results: Overall, 8 in 10 PCPs reported child mental health is a significant problem in their community and 67% are much more concerned compared to before the pandemic. Caring for children with mental health conditions was commonly reported: 26% and 21% see patients with anxiety and depression, respectively, every day; 20% and 16% see children with suicidal ideation/behavior and eating disorders, respectively, about once a week or more. One in 4 PCPs said it is very difficult to find care for patients. Most (76%) prescribed psychotropic medication in the past year. Less than 1 in 10 of those prescribing was very comfortable doing so. Several variations were found by practice area (Table). For example, rural PCPs were most likely to report resources are not at all available (20% vs 4-5% in other areas; p<.001), and prescribing was more common in rural (88%) and suburban (82%) than urban (71%) and inner city (61%) areas; p<.001.
Conclusion: Most PLACES primary care pediatricians have significant concerns about child mental health in their communities and many see children with anxiety and depression daily. Findings underscore the continued lack of mental health resources in rural areas and a need to better support pediatricians prescribing psychotropic medication.
Table 1. PLACES primary care pediatricians’ views on and experiences addressing child mental health needs by practice area, 2022
Last Updated
05/22/2023
Source
American Academy of Pediatrics